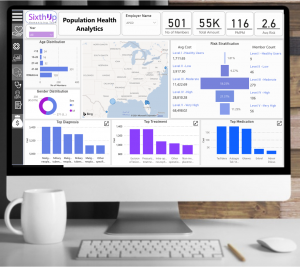
SixthUp Announces Launch of the Healthcare Analytics Solution for Benefits Consultants, Brokers, Payers, and Employers
The Solution will help understand the latent risk in the population while improving the health outcomes and optimizing costs.
PLEASANTON, CALIFORNIA, UNITED STATES, January 10, 2022 /EINPresswire.com/ -- SixthUp, a US-based consulting firm that provides cloud services, emerging tech, and digital journey transformation solutions across a range of industries, including Healthcare, announced the launch of its healthcare analytics solution.
The healthcare analytics solution enables benefits consultants to gain a competitive advantage by increasing benefits engagement for their clients. It allows them to propose innovative solutions to improve their clients’ benefits strategy and achieve higher employee satisfaction scores by:
1) Tracking employees with chronic conditions and monitoring their medication cost & utilization patterns to predict the cost of employee benefit
2) Forecasting financial resources based on employees’ risk factors
3) Engaging employees in early preventive care and planning stop loss & reinsurance coverage by identifying and targeting high-risk employees
The solution allows payers to leverage data and analytics to make informed decisions on risk coverage, utilization, and spend, by utilizing features such as:
1) Member Cohorts Analysis to dig deeper into the health data
2) Predictive Analytics to help identify members’ risk factors that may contribute to hospitalization and high costs of care
3) Performance Tracking and Comparison of various benefit plans using claims, enrolment, and utilization analysis
4) Automated Data Ingestion Pipeline using FHIR standards
5) Custom Interactive Reports and Dashboards to build scenarios and view possible outcomes
Ashish Choudhary - CEO, SixthUp, states that - “Healthcare analytics and data-driven technology are being increasingly accepted as the way forward by the players in the healthcare industry, and are being used more widely to improve benefits strategies, predict risks, cut costs and improve the quality of patient care. However, a majority of payers and benefits consultants fail to leverage these technologies and struggle with day-to-day challenges and inefficiencies. SixthUp’s Healthcare Analytics solutions are meant to help these players overcome their challenges and enable greater efficiency, financial viability, and enhanced outcomes.”
Sanjay Saini - Practice Head at SixthUp, says - “The second largest cost for doing a business after salaries and wages is employee benefits. Still, most employers are wasting resources and money on plans employees are not utilizing. Each year, about 18% of rising-risk patients escalate into the high-risk category when not managed. Greater than 60% of high-cost members in any given year were not there the previous year. SixthUp’s Healthcare Analytics solution has been designed for Employers, Brokers, Benefit consultants, and payers keeping these very challenges in mind enabling them to drive benefits decisions and optimize costs.”
SixthUp’s suite of offerings includes cloud, data, analytics, AI and machine learning, web application development, automation services backed by accelerators for digital journey transformation, data analytics, and insights.
About SixthUp
SixthUp is a technology consulting firm that provides emerging tech, Cloud, and Digital services to fuel our client’s business growth. Our approach eliminates risk, accelerates our client’s time to market, and enables them to reap the true reward of embracing the tech. SixthUp represents Dynamic Technologies group, which has been providing technology and software solutions for more than two decades to organizations across industries in the US, Europe, and Africa.
Media Contacts
Shilpa Tandon
SixthUp
+1 925-315-9897
email us here
Visit us on social media:
LinkedIn
Legal Disclaimer:
EIN Presswire provides this news content "as is" without warranty of any kind. We do not accept any responsibility or liability for the accuracy, content, images, videos, licenses, completeness, legality, or reliability of the information contained in this article. If you have any complaints or copyright issues related to this article, kindly contact the author above.