The Mobil-Aider Takes the Guessing Out of Joint Assessment
An Innovative Device Funded by the National Science Foundation
SPRING CITY, PENNSYLVANIA, UNITED STATES, May 15, 2020 /EINPresswire.com/ -- The Mobil-Aider is an innovative orthopedic device that permits clinicians to address a “pain point” through the quantification of joint linear translation (Figure 1). This impacts the ability to accurately assess joint injuries and provide consistent, efficacious treatments to enhance injury recovery. As a first to market device for these tasks, the Mobil-Aider will allow the development of a body of knowledge that is significantly lacking.
Quantifying joint mobility/laxity is a challenge for clinicians. Assessing millimeters of motion qualitatively is not reasonable. Studies have reported that skilled clinicians have good relative intra-clinician reliability, i.e. they could replicate their “linear translation” during joint assessment and mobilizations, but had poor to moderate reliability between clinicians. In other words, clinicians are not in agreement when it comes to quantifying joint mobility/laxity. This is a problem. In a discipline like orthopedics that prides itself on precision, we should be able to do better than state a joint “feels lax” or “feels tight.” The Mobil-Aider has emerged as the transformative device to address this clinical issue, both as an examination and a treatment tool.
In terms of examination, injury to the knee anterior cruciate ligament (ACL) is assessed dynamically with a Lachman test or statically via Magnetic Resonance Image (MRI). Despite the Lachman test being widely accepted, there are several reasons for a high number of false negative results with ACL testing. First, faulty test positioning (too much knee flexion) and hamstring muscle guarding can prevent anterior tibial translation. Second, test results are dichotomous: positive if the ligament is torn and negative if it is intact. Issues arise if the ligament is partially torn or stretched? Guillodo et al (2008) found the misdiagnosis of acute ACL injuries by emergency room physicians to be 74%. Finally, asymmetry greater than 3-5 mm in side-to-side laxity or a soft endpoint is considered abnormal. Even the most experienced clinician can find 3 mm extremely challenging to quantify. Furthermore, MRIs only provide a static image of the ACL condition. They do not provide information about biomechanical behavior of the ligament so the ability to identify partial ACL tears has been called into question. The Mobil-Aider can assist the user in mitigating these issues (Figure 2).
Regarding treatment, performing consistent joint mobilizations begin with the way the task is learned in the classroom. One can appreciate the cognitive elements of mobilization grades, but unless this knowledge is transitioned to the psychomotor skill, it is of little value. The mastering of the psychomotor skill requires purposeful practice with feedback, specifically, concurrent, visual feedback. The key innovation associated with the Mobil-Aider is the ability to quantify the magnitude of joint translation. The light-weight, versatile, and cost-effective device uses LED feedback to provide real time quantification of the linear translation. The device design permits classic joint mobilization techniques, thus minimizing the learning curve for the user. A variety of specifically designed attachments permit the use of the device for the shoulder, elbow, wrist, knee, and ankle (Figure 3). The goal of quantifying feedback is to increase consistency of joint mobilizations to enhance the patient outcomes.
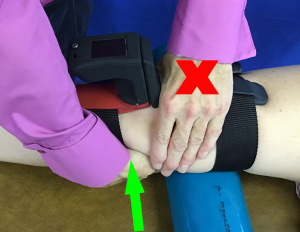
To use the Mobil-Aider, the clinician interfaces the device between the patient’s skin and the clinician’s hands. Aside from knowing which attachment to use, no additional training is needed to quantify the linear translation of a joint. The clinician obtains a quantified (digital) read-out while also appreciating the qualitative endfeel. The ability to see instantaneous digital feedback could be extremely valuable to the training of emerging clinicians and enhancing the consistency of seasoned practitioners.
Data regarding reliability and validity has been published in three peer-reviewed journals. To summarize the bench data, Pearson correlation coefficients ranged from 0.986 to 0.997 and Cronbach’s alpha was 0.992 to 0.997. In addition, a case report comparing the Mobil-Aider with radiographs of the knee when performing a Lachman test yielded a margin of error of just 2%. This is promising given prior research on the KT1000 revealed margins of error up to 28%. Additional clinical research needs to be performed and it is currently underway.
Note: The Mobil-Aider was invented by Dr. Dawn Gulick and has been funded by the National Science Foundation and Ben Franklin Technologies. The device has been approved by the FDA as Class 1 exempt and the patent is pending.
For additional information visit: https://iortho.xyz/mobil-aider/ or email: info@iOrtho.xyz
Dr. Dawn T Gulick
Therapeutic Articulations, LLC
+1 610-570-7153
email us here
Visit us on social media:
Facebook
Twitter
LinkedIn
Mobil-Aider NSF Video on 3-Pain Points of Knee Testing